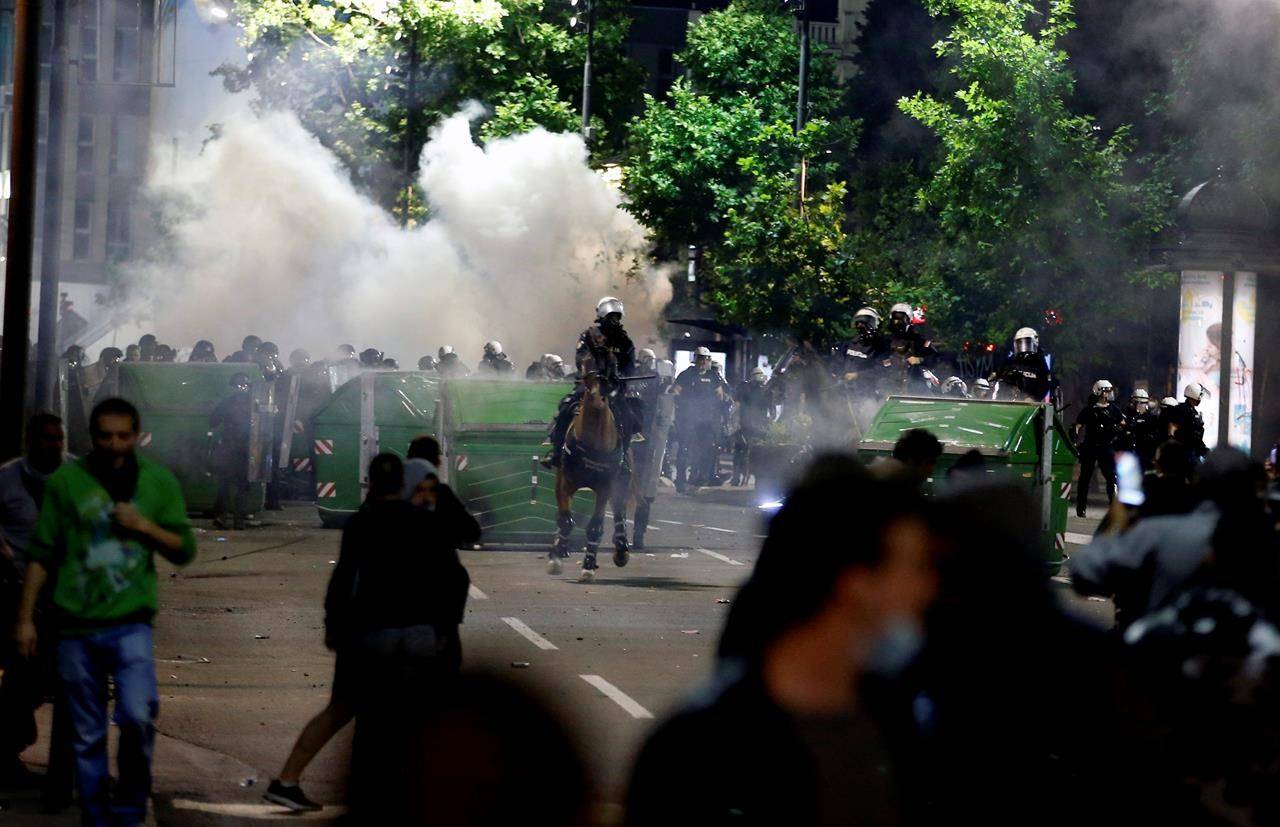LOS ANGELES — For two weeks, Rachael Jones has stayed home, going without a paycheque while waiting and waiting for the results of a COVID-19 test from a pharmacy near Philadelphia.
“I’m just so disappointed. I just don’t know how — with the resources and the people we have and the money we have — we can’t get this right,” she said.
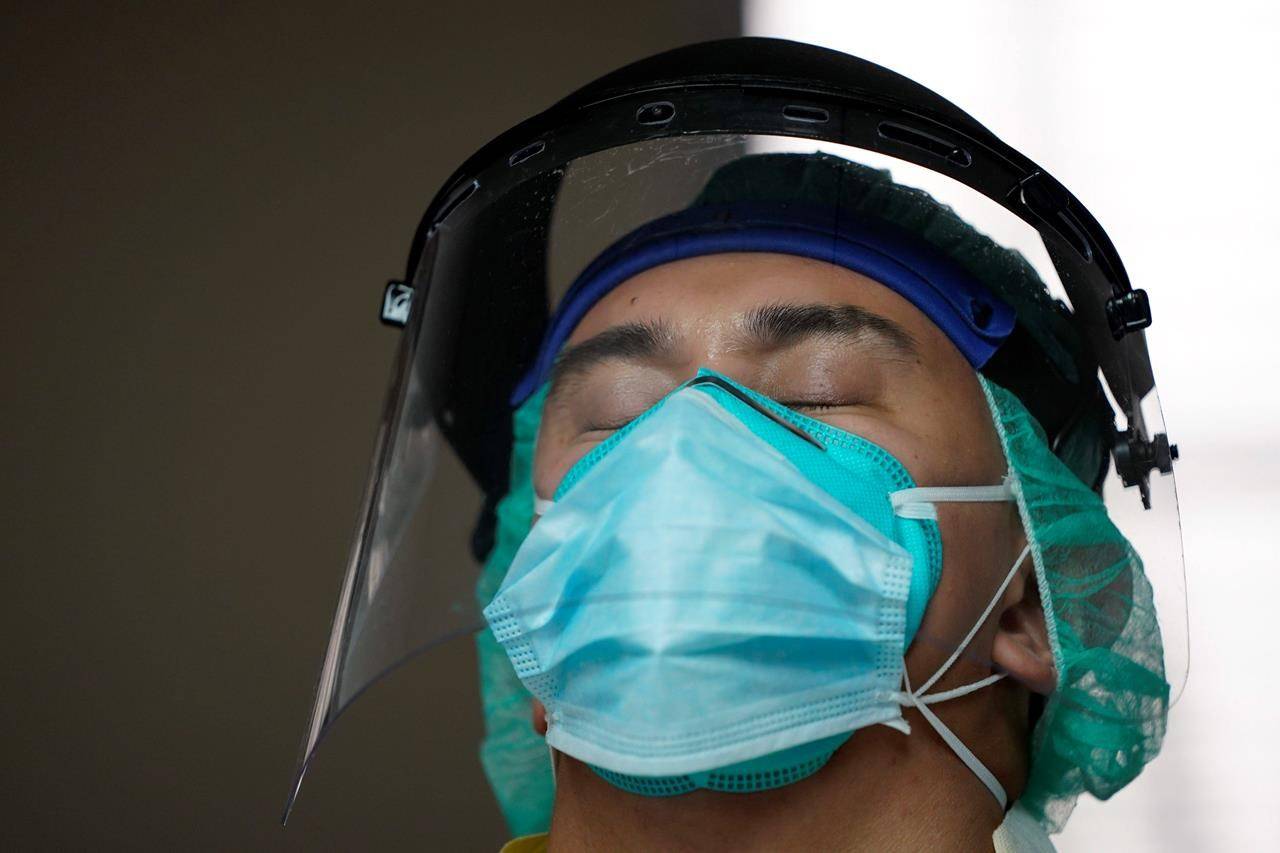
Four months, 3 million confirmed infections and over 130,000 deaths into the coronavirus outbreak in the U.S., Americans confronted with a resurgence of the scourge are facing long lines at testing sites in the summer heat or are getting turned away. Others are going a week or more without receiving a diagnosis.
Some sites are running out of kits, while labs are reporting shortages of materials and workers to process the swabs.
Some frustrated Americans are left to wonder why the U.S. can’t seem to get its act together, especially after it was given fair warning as the virus wreaked havoc in China and then Italy, Spain and New York.
“It’s a hot mess,” said 47-year-old Jennifer Hudson of Tucson, Arizona. “The fact that we’re relying on companies and we don’t have a national response to this, it’s ridiculous. … It’s keeping people who need tests from getting tests.”
It took Hudson five days to make an appointment through a CVS pharmacy near her home. She booked a drive-up test over the weekend, more than a week after her symptoms — fatigue, shortness of breath, headache and sore throat — first emerged. The clinic informed her that her results would probably be delayed.
Testing has been ramped up in the U.S., reaching about 640,000 tests per day on average, an increase from around 518,000 two weeks ago, according to an Associated Press analysis. Newly confirmed infections per day in the U.S. are running at over 50,000, breaking records at practically every turn.
More testing tends to lead to more cases found. But in an alarming indicator, the percentage of tests coming back positive for the virus is on the rise across nearly the entire country, hitting almost 27% in Arizona, 19% in Florida and 17% in South Carolina.
While the U.S. has conducted more tests than any other nation, it ranks in the middle of the pack in testing per capita, behind Russia, Spain and Australia, according to Johns Hopkins University.
Testing alone without adequate contact tracing and quarantine measures won’t control the spread of the scourge, according to health experts. But they say delays in testing can lead to more infections by leaving people in the dark as to whether they need to isolate themselves.
Thailand, South Korea and Norway, among other countries, have controlled the virus more effectively while conducting fewer tests per capita than the U.S., according to Johns Hopkins.
In other developments:
— While the number of confirmed cases in the U.S. hit 3 million Wednesday by Johns Hopkins’ count, health officials have said that because of inadequate testing and the many mild infections that have gone unreported, the real number is about 10 times higher, or almost 10% of the U.S. population.
— Most New York City students will return to school in the fall two or three days a week and learn online the rest of the time under a plan announced Mayor Bill de Blasio. He said schools can’t accommodate all their students at any one time and maintain social distancing. The school system in New York is the biggest in the nation, with 1.1 million students. It has been closed since March.
— In Serbia, lockdown measures touched off violence that left at least 60 police and protesters hurt in Belgrade. Protesters tried to storm Parliament and set fire to five police vehicles.
— Spain said the daily infection count doubled in 24 hours amid dozens of small outbreaks. Romania and Iraq recorded their highest daily totals yet. And Australian authorities planned to lock down the city of Melbourne for a second time because of a spike.
The U.S. Department of Health and Human Services this week said it will open free “surge testing” sites in three hard-hit cities: Jacksonville, Florida; Baton Rouge, Louisiana; and Edinburg, Texas. The sites will be able to conduct as many as 5,000 tests a day in each city, with results in three to five days, officials said.
In Georgia, one of the states where cases are surging, officials are rushing to expand testing capacity as demand threatens to overwhelm six major sites around Atlanta, said DeKalb County CEO Michael Thurmond.
“If you project this out over the next three weeks, we can’t handle it,” he said.
In New Orleans, people were turned away from a free testing site for a third consecutive day after it reached its daily allotment of tests. Health care providers are running low on trays and chemicals needed to run machines used in the tests.
Phoenix Mayor Kate Gallego called the situation there “desperate” as residents have sat in sun-baked cars for up to 13 hours to get drive-thru testing. Robert Fenton, head of the Federal Emergency Management Agency, said FEMA is doubling the testing supplies it plans to ship to Arizona.
Patrick Friday, a United Methodist minister in Alabama, went to several hospitals and clinics in Birmingham this week to get checked after his school-age son tested positive. But he was told that unless he had a preexisting condition, he didn’t qualify.
Finally, he ended up at a site offering rapid-result tests and his negative result came back quickly.
“We are several months into this,” he said. “How can it be that we can’t go in and get a test?”
___
Tulp reported from Leawood, Kansas. Associated Press reporters from around the world contributed to this report.
___
Follow all of AP’s pandemic coverage at http://apnews.com/VirusOutbreak and https://apnews.com/UnderstandingtheOutbreak
Christopher Weber And Sophia Tulp, The Associated Press